10. Might we better try to map COVID-19 across space and against the limited public health services and resources we have? We were told rates of hospitalization for COVID-19 would peak in mid-April across the United States, and a peak in the mortality for the global pandemic in the United States was announced to be on the horizon. But a third of the world’s cases of infection lie in the United States, and we still have an inadequate national model for testing,–even as we are transitioning to a policy of “opening up” states formerly in lockdown or Shelter-in-Place (SIP) states, also know as Stay at Home or other euphemisms that fail to describe the states we are actually mentally in. In California, the deadliest day so far from the novel coronavirus was, however, yesterday. But as numbers of infection that were never counted in a reliable manner testing could have provided–or that preparation of a proper test kits for the SARS-CoV-2 virus would guarantee–rather than follow any models that were predicted, we seem to be at a stable line of 30,000 infections as some global tallies have begun to fall–perhaps due to mortality–and some, as India, seem still to rise.
Perhaps the most accurate map of its spread over space is not a spatial map at all, but the phylogenetic map of SARS-CoV-2 as the pandemic has expanded globally across six continents–if, thankfully, not to mutate drastically, although we have been tracking the spread of the virus primarily through numbers of infected–or tragically killed–in maps of political boundaries.

Although there is a terribly compelling self-interest in regarding any map of COIVD-19, a self-interest that seems to have allowed us to bracket, in the United States, the location of the novel coronavirus outbreak in China, as increasing numbers were infected in December to January, as we focussed in the United States on the extracting of nationals exposed to the virus, we turned to “community-based surveillance” to track the virus in human communities to be vigilant for “hot-spots” as they appeared, rather than coordinating national testing, as the network of COVID-19 grew across space, far beyond current mapping or tracking tools. “You can’t stop it, if you’ can’t see it,” warned the World Health Organization’s Dr. Bruce Aylward, and while testing was absolutely vital to track the highly communicable virus, and the lack of expertise in organizing a response from either CDC director, Dr. Robert Redfield, who specialized in addiction therapies; the absent infrastructure to manage the disease outbreak terrifyingly left the nation without any adequate maps to come to terms with the disease.
We lacked a sense of the narrative of this spread, of course, and were not ready to link the proliferation of data to an interpretation of the virus’ rapid spread. Even as we were barraged by maps, as the benificiaries of new location technologies, that have helped facilitate and improve the provision of maps, even if based on bad data, they were produced at a disconnect from the lack of official response to the disease.
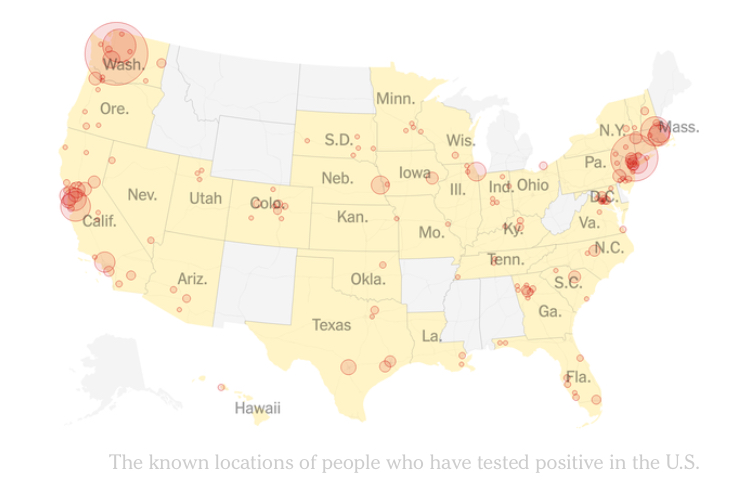
We tried to follow the virus by cumulative tally of deaths–a shocking metric, a tally we have yet to try to get our heads around and packs a tremendous punch–seems reserved for other periods. But if the worst-case scenario has been avoided, with over 53,000 dead in our country–the difference from the 2.2 million deaths forecast for the United States if the spread of the virus was unchecked, leading to discussion of an approaching, if qualified “re-opening” of the nation, as screening is multiplying–but COVID-19 “hotspots” have spread across the entire eastern seaboard, in a visualization that reveals the broad compromise of our public space. The epistemological distancing of much of the nation from “coastal” communities, disturbingly evident in the 2016 election of President Trump, was eerily mirrored in the rise of outbreaks of infection and mortality across the nation from COVID-19, leading many governors and many Trump supporters to distance themselves, refusing to wear masks the might reduce communication of the novel coronavirus that had revealed rates of infection and low immunity. Most problematically, we were mapping in national terms a crisis that was global, and demanded a type of global mapping we are not able to process or grasp.
As the virus COVID-19 was not named before February 11, soon before the first fatalities in France and Italy on Feb 15 and 21, both of elderly, the rate of infection of what would be called a pandemic had no clear mapping strategy until it had become a global pandemic, already on four continents, in March 9 we focussed on the paucity of cases outside the coastal areas, believing the disease could be contained, even as the numbers reported were far lower than the number human hosts who had contracted the virus, or had communicated it to others.

We focussed on the arrival of a cruise ship in Oakland that had docked, carrying COVID-19 patients, in the nearby harbor, but were shocked when we talked to folks on the east coast urgently telling us to cancel cross-country trips at all costs.

In a case of the tragedy of dislodging the map from the legend, or allowing the map to embody meaning, we were left without any sense of a global narrative, or any narrative structure to read the data that was displayed in maps, preferring the human drama, perhaps, of the passengers who had found safe harbor in Oakland, to be spirited away to military hospitals in Davis, CA, and elsewhere, and no global narratives to discuss the migration of a pandemic disease, let alone one that turned out well.

The rates of infection that have hardly been able to be contained makes us pause, however, and fear the ravages of the nation that COVID-19 has left behind, both candidates for the highest office in the land no doubt getting tested once or twice a week, as testing is lacked for much of the country, an absence in availability that no doubt reflects the distance of much of the nation from institutions of health care–
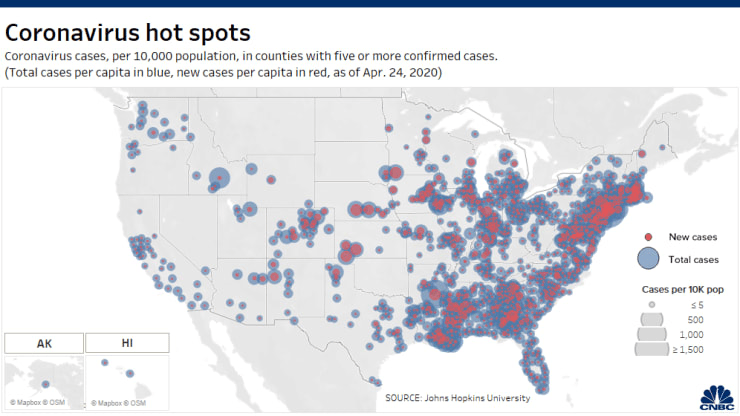
–but which deny or obscure the global nature of the disease, or even the signs that the disease presents itself globally as a pandemic, rather than in terms of nations or states. Perhaps it is more opportune to map the migration of the pandemic on March 10–just as it was gaining that name, far later than should have been the case–show in the distinct strains of COVID-19 arriving in the United States from both China and from Europe.

Much as strains of zoonotic diseases are apt to spread from host species in certain global regions, where the leap from mammal to human hosts are most likely to occur, the prevalence of hot-spots of the likelihood of such transmission have suggested attention to the probability of greater and lesser reservoirs of pathogens across a global spectrum, the high level of sites of pathogenic leaps in specific sites, might help to create a preemptive map of zoonotic outbreaks, the mapping of susceptibilities to disease outbreaks, transmission, and cannot be limited to global travel,
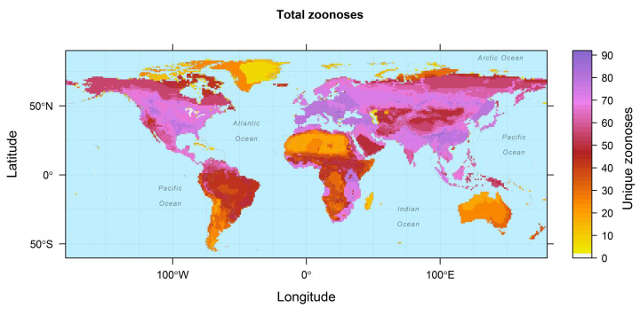
But we map them, tied to statistical models that propose a legible vision of the state, to map their outbreaks as if bound by national confines, or as specific to individual states. The dangers of so doing might be less valuable, and more deeply distorting, than we want, however difficult it is to ask readers to focus on an illness’s global dispersion as of relevance to themselves.
During this national emergency, we are experiencing both a stress test for the nation–is a global health crisis. We have watched since January illness and rates of infection advance across the globe on our maps suddenly was moving in waves across the nation, as what was a burgeoning problem for Chinese health authority swung global, in ways we somehow didn’t expect–even if we new all things came in global sizes today–cutting down borders, improvising unhelpful quarantines, imagining that a reassuring sense of symbolic security could continue to be retained in the face of COVID-19.

We were asked to focus on the virus epicenter, in the earliest maps, a misleading metaphor from an earthquake, ample in describing its global scope, failed to describe its difficulty to map or track. But does this make sense to describe the spatial spread of the virus that replicates itself over time and space, traveling in human hosts across national borders, and even continents? The seismological term “epicenter” amplifies confidence to our mapping skills, but the spread of COVID-19 occurs without relation to a site, and eludes the very sort of objective mapping a seismologist is able to pinpoint: the destructive migration of COVID-19 is less able to be pinpointed with meaning, if it suggests a deep problem of plate tectonics in how it stands to transfigure our sense of place.
But national maps processed an overwhelming amount of data of exponential growth about the presence of the virus in human hosts, offering an uneasy hold on the spreading contagion. They did so not by embodying it–as might be true for the classical maps of infection, from John Snow’s mapping of cholera around a single pump’s handle in London’s Soho neighborhood, in 1854, using military maps to come to terms with the invisible spread of pathogens, and orient them in space about a single site of infection that could be removed to contain the clustering of deaths: but the viral spreading only revealed our inability to grasp the rapidity of its contagion across space in a globalized world.
Cholera, the first disease whose contagion was mapped in detail, was, much as COVID-19, a pandemic that spread globally, migrating from 1832-33 with people, on ships, and in caravans across much of the first half of the century, and demanded to be contained in similar ways in cities: but the velocity of the spread of COVID-19 across the globe was a newly emerging disease that jumped space in ways our maps didn’t concretize in a graspable manner. But the spread of COVID-19 responded in proportion to the scale at which the rural environments were disturbed at one site, that cascaded globally across the world, knowing no national or regional bounds–as much as we continue to map it in national terms.
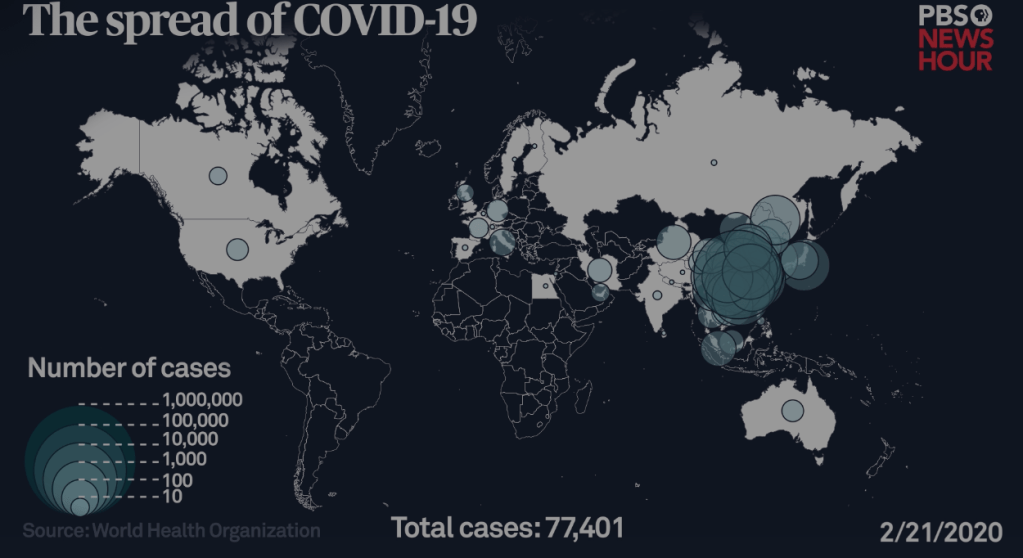

We don’t map the zoonotic nature of the virus, or how it jumps from one species to humans, if only because our maps of its spread affirm the illusion of a control over nature, and the separation between nature and human society that all maps seem to affirm. We may even hold onto maps as the only means to have any security about this novel coronavirus and its relation to the world, but are finding that the inadequacy of any simple map to process the progress of the disease reveals the lack of authority of the superabundance of maps to contain or conceptualize the disease–as it spins out of our control.
These global maps are clearly not enough. For while they do track confirmed outbreaks, whatever the accuracy of such “confirmations” are, such maps are inadequate as sites for orienting us, if they give a clear and crisp sense of purchase on an unfolding global scenario. For the maps offer no sense of an epistemic purchase or breakthrough to understand infection, of a virus able to be communicated across airborne mediums, or even cultivated in man-built structures, as hospitals, airplanes, theaters, or marketplaces, the demand for orienting viewers to its spread a cottage industry of visualizations that we watch as we do what we can only do–watch the scope of the viral infection expand as observers of the observed.
The maps reflect a breaching of a barrier between nature and culture, or human society and a virus living in forests, but they hardly orient us to that breach. They suggest the only way we can reduce its spread is by slowing the pace of frenetic global movement of human bodies–as we struggle to shelter in place. Maps can seek to stabilize its spread. But the jump of the pathogen from forests to the urban slums in Hubei province ricocheted across species in ways that revealed a set of interconnections among global populations in infections that reveal an intensified spatial continuity we can’t circumscribe or bound with any confidence, if the range of maps produced about its spread are testament to how very desperately we want to do contain the spread of a virus that we can only be the global spectators of, now that it has, as the Center for Disease Control (CDC) tells us that over three quarters of “new or emerging diseases” to which we are so vulnerable, as SARS-CoV-2, infect humans from wild or domesticated animals. But we looked at these maps, as if conditioned by GPS, which will alter our ways of reading maps forever, the scariest aspects of cartographies of COVID-19 is how universally the spread of a pandemic over global space are read as revealing the inability to escape disease–from Amitav Ghosh to Orhan Pamuk–as it grows.
There is an unabashed egotism in consuming maps of the disease that orient us to when the infections will “peak” in different states, without understanding the different nature of epidemics and strains of SARS-CoV-2 in different regions, and the inability to chart the pathogen’s progress only in relation to human life, or without acknowledging its currency in man-made environments that encouraged the zoonotic disease to jump into the built webs of a human world. In tracking the progress of the disease as spatial, and of degrees, we can, in a sense, to claim mastery over it–asserting some level of understanding we may still have, and obscuring by the need to imagine the stability of the static terrain of a nation concealed how a shifting global ground allowed the zoonotic virus to jump species and the novel coronavirus spread.
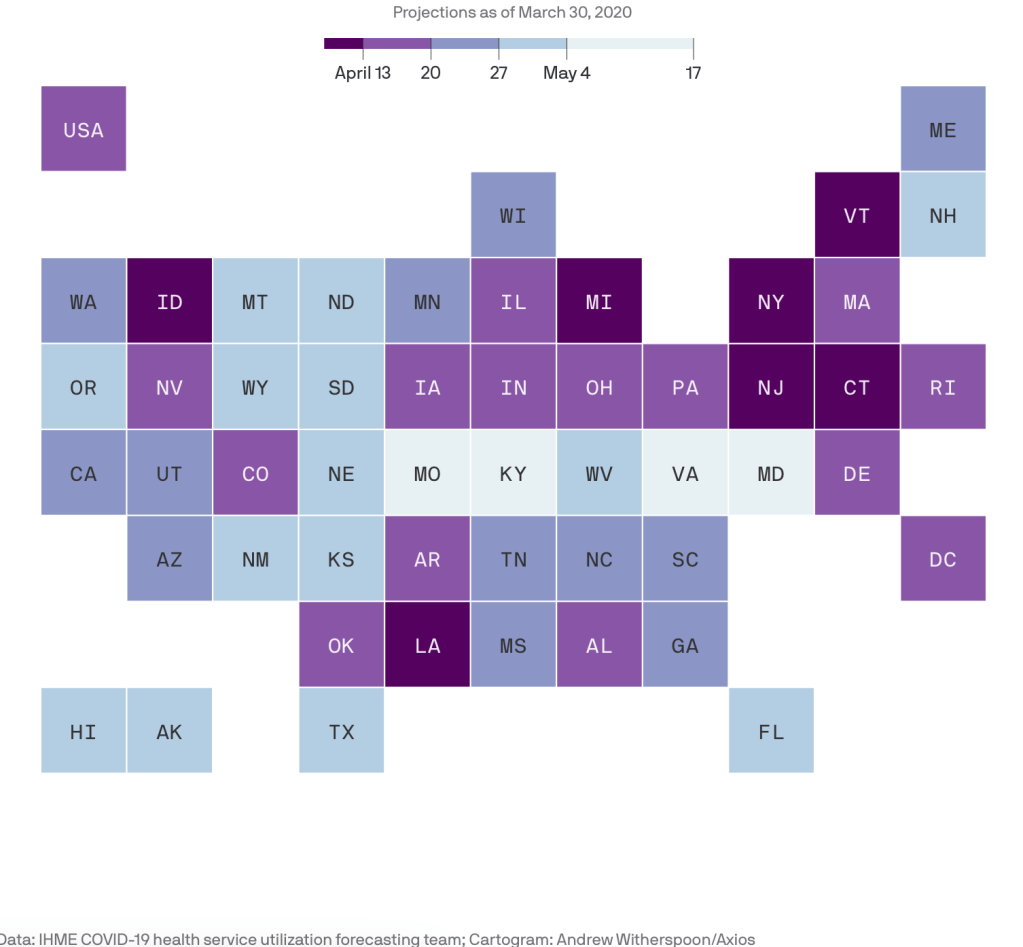
National maps suggest an ability to contain the spread of the virus and orient ourselves to it. And while the spread of the virus cannot be contained, we try to flatten the curve, as if to bolster our sense of being able to control its spread, and to adopt the only measures we know of curtailing its circulation in the air and contraction across our increasingly shared spaces of life. But the problems of mapping the virus are acute, and suggest the need to include tables, graphs, and charts among our COVID-19 visualizations,–as we increasingly depend on them for all maps, as Bill Rankin has argued, even if we use Web Mercator–as if to familiarize the spread of a virus that is so unfamiliar and so unknown.
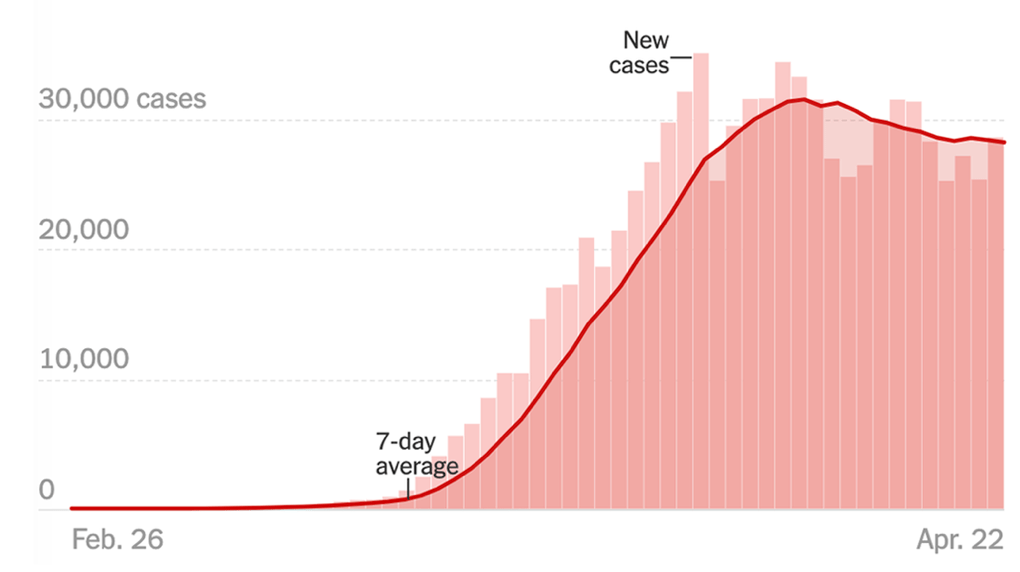
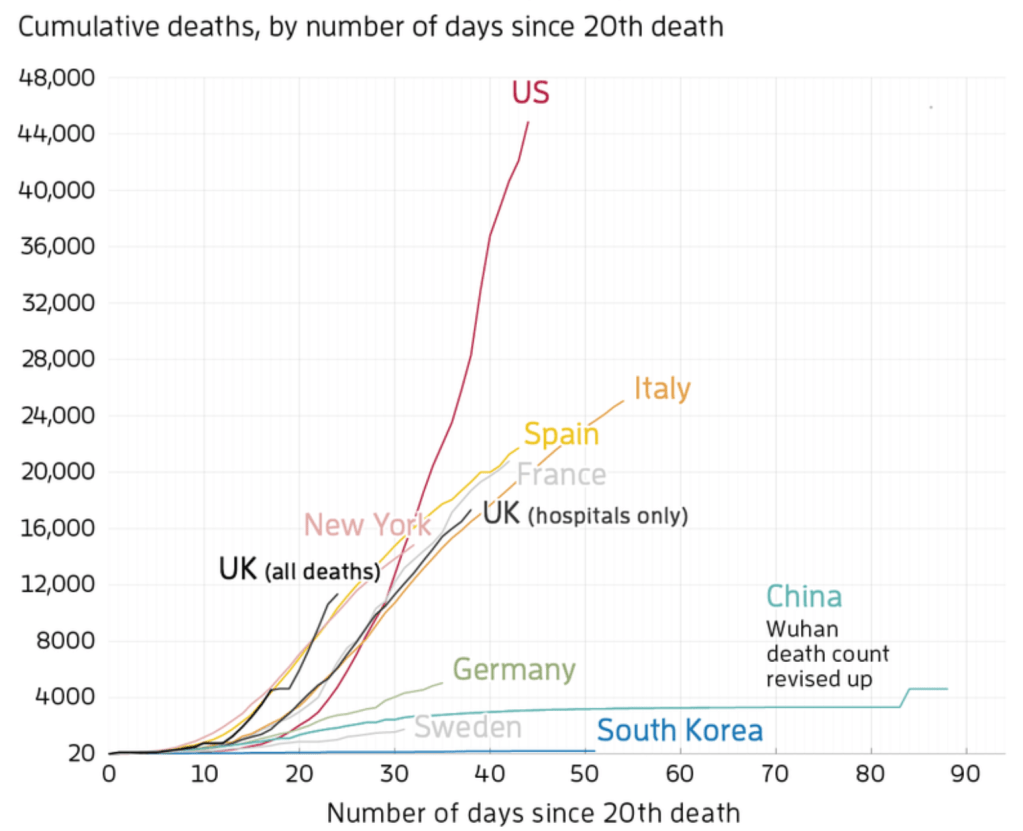
The simplification of its spatial progress is of limited predictive value–save for the immediate need of hospital beds. The “maps” of infections, cumulative or daily, or rates of mortality, have a funeral drum-like aspect of an existential fatalism, where we are watching the progress of the virus through human bodies, in ways impossible to process and even less possible to give us a sense of agency. So clearly do the maps of the spread of COVID-19 suggest the miasmatic spread of an illness that cannot be controlled, as if noxious vapors carry the airborne virus into alviolae, we might well return to the images not of miasmatic infection, but awaiting a sense of grace–of medical practitioners who pose themselves to infection, of the evidence of a lack of influence of warming weather on the disease, and of continued hope for the arrival of a vaccine: clinging to hopes is characteristic of how passions overtake reason in a plague.
11. We can only seek a moment of grace before the onslaught. The search for a moment of grace, an epiphany of insight as in Michelangelo’s Pietà, an emblematic moment of mortality restaged for COVID-19: the famous marble block of sculpture a young Florentine carved for the funerary monument, for a socially climbing French cardinal, eager to create a lasting memento to human mortality, has become the only way we can see the body of the novel coronavirus patient, no longer able to be kept at a distance, but presenting an image we all unavoidably need to understand, a drama that is the central overwhelming global drama of attempt at health care that blends with a sense of shared mortality, a single case or moment concretizing the national tradition and national sense of collective action and collaboration, a hope for the combined draw of physicians, medical nurses, and clinical collaboration, with a respirator applied to the patient, their body held by attendants in full protective garb, and a man who reaches out exposed arms to help the elder patient who struggles silently, in need.

This is, of course, both a national icon of care and attention, and a new refiguration of a modern concept of medical service–an old drama being played out in new roles, to be sure, in a sort of cross-dressing across the ages, that is the eternal drama of life and death. In emulation of the tomb statuary Michelangelo had designed for a French cardinal concerned with the fate of his soul, we search for a new model of being, or at the very least new Art of Dying, shifting from hopes for awaiting immunity or antivirals to a basic need for some consolation of our mortality. Or is the message indeed deeper in repositioning of a familiar topos of mortality, as a search for the possibility of a grater sense of transcendence in a crisis of mortality of dimensions and scope that seem outside the modern era?

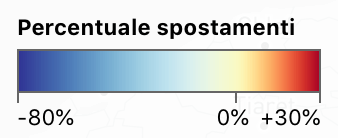
We are only, in the end, “human, all too human”–but is there a comfort, akin to the signing out of operatic arias from balconies while sheltering in place and keeping social distance, of a rediscovery of a common core or culture of humanity? Such a sense of comfort, indeed, stands at a remove from the fear of dislocation from the past, and from tradition, or from normal life–whatever that is!–that is posed by the coronavirus, in response to which mobility across the entire Italian peninsula has suddenly, and so unfamiliarly, paused with the expanse of infections, measured by province and region below, and imagined as a new Ice Age by the clever folks at Terralytics, inviting us to reckon the consequences decreasing all movement by up to 80% across the peninsula–an image to which this post will return, of the immobility of movement across all regions of the peninsula that registers the impact of the coronavirus, as a moment when time and space merge.

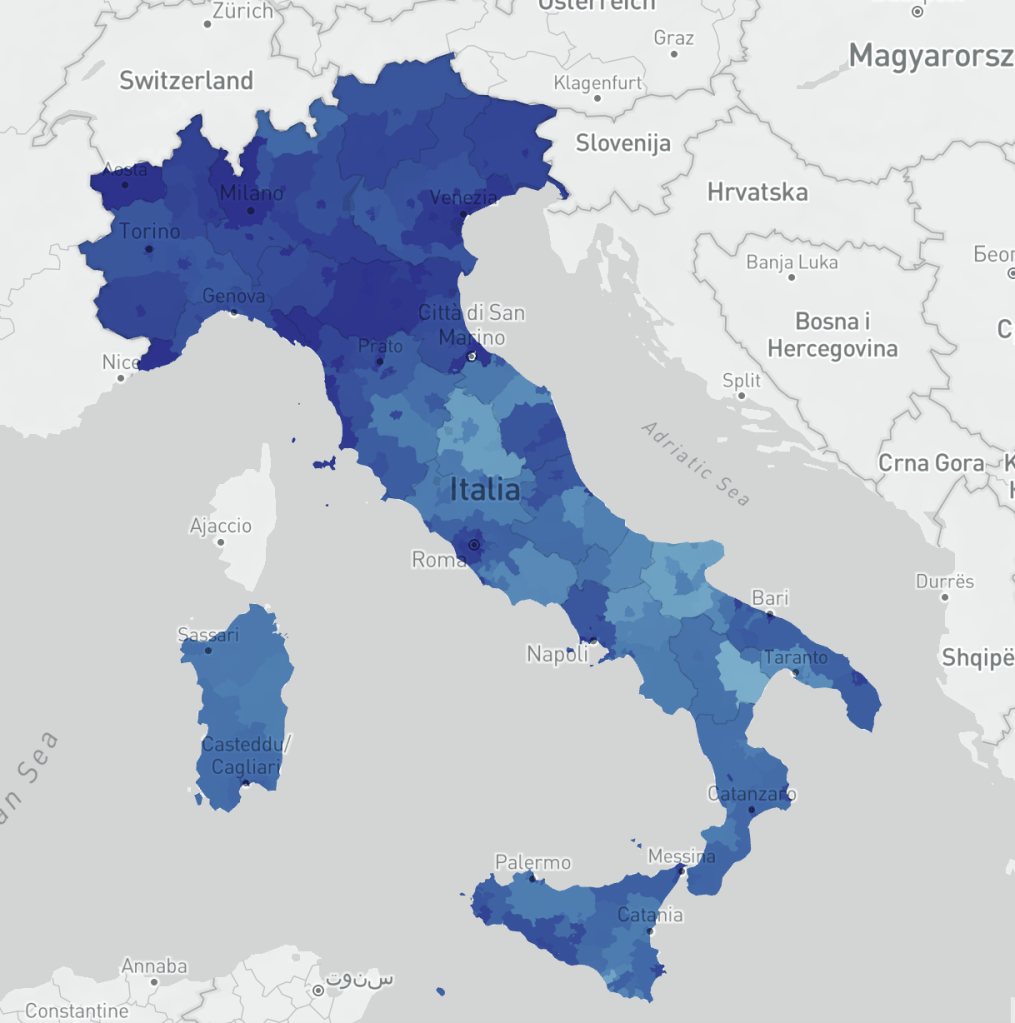
Teralytics, (c) Mapbox, data (c) OpenStreetMap
Are we, too, frozen before the drama of health care continuously enacted around us, in our buildings and neighborhoods, of those we love, and seems as if it englobes us. We are in the course of it all trying to preserve a sense of compassion–and a pressing sense of mortality, and timelessness, despite all modern medicine, or mapping techniques of data aggregation. We cannot map ourselves in relation to this illness, its incubation periods, its infection from asymptomatic bodies, the incomplete tallies or testing of infections that move through bodies, against the brunt fact of the mortality of the human body we have not liked to keep so much in the open, or so visible and ever-present in our world, but is now terribly made more immediate than in recent memory.
Or might we find a more human, and indeed more meaningful, reaction to COVID-19, by looking at the early work sculpted from marble by an adolescent Michelangelo, over almost five centuries earlier? It seems a search for a sense of transcendence, a moment of reprieve in the massive onslaught on mortality we can be expected to find difficult to process.


Were we all being asked to come to terms with the immediacy of a new “art of dying,” to come to terms with a dizzying rush of statistical tabulations of mortality rates we can barely comprehend, as an outpouring of obituaries filled pages of local northern and southern Italian towns’ newspapers, challenging one’s ability to process, even as we need new benchmarks to move ahead?
Yet we returned to cleaning spaces, social distancing, and mitigating the communication viral loads, learning masks, and protective uniforms, as we hoped to staunch the virus’ spread and the threat that it posed to all.



It is amazing that his response is to close the borders. Has to be something weirder than denial, as you suggest. Border closing as both cause and “cure”.
The denial seems cognitive, but inability to acknowledge the responsibility of governments suggests a stunning lack of prioritizing public health safety. The script of demonizing foreign countries was on auto loop, and the world will suffer!